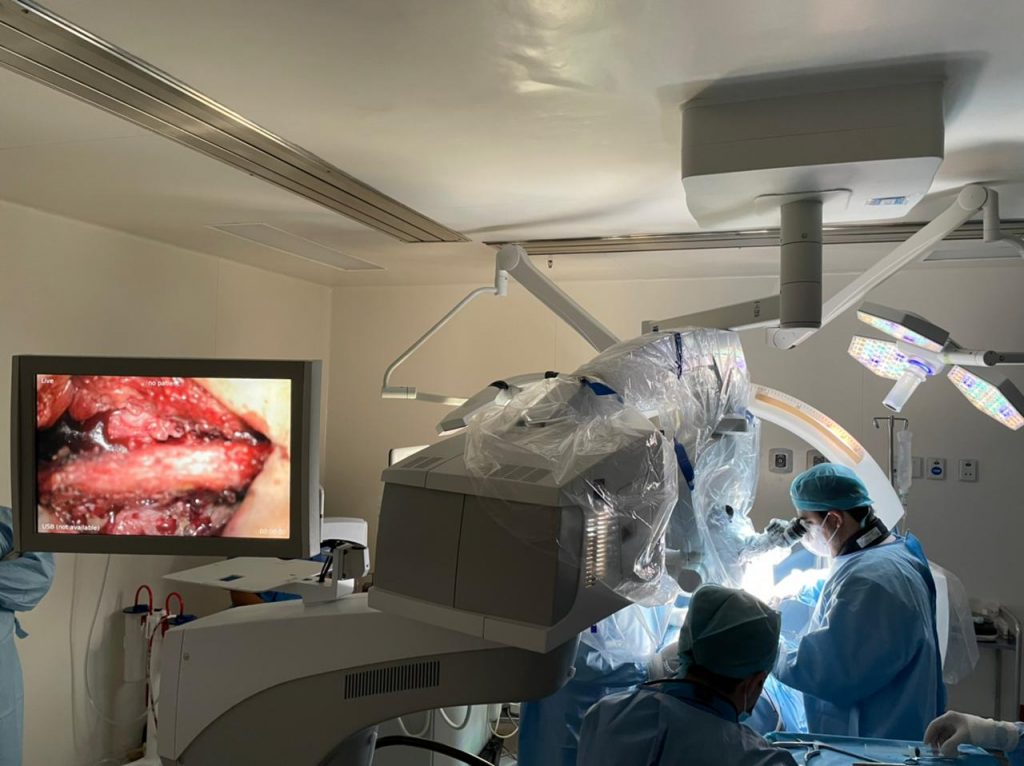
Endoscopic spine surgery (ESS) is currently considered the most obvious example of evolution that this specialty has had.
The incision is made in less than one inch in length. It is even possible with older patients, those who are at high risk when using general anesthesia, and in some cases, anesthesia blockage can be performed to give the patient regional anesthesia.
In endoscopic spine surgery, tubular retractors minimize the need to cut soft tissue such as skin and muscle. The recovery is less cumbersome for the tissues. Consequently, there is less blood loss and better patient recovery.
Endoscopic spine surgery is performed even faster than open surgery. You should consult with your specialist which is the best surgery depending on each condition, since the same condition can be addressed with any technique, but the experience and skill of your specialist determine which is the best for you; particularly considering second surgeries, spinal instability, high grade spondolisthesis and cancer.
First step of the surgery is the incision and it will fit a tubular device about the thickness of a pencil to be inserted. A camera is inserted into this type of cannula with the ability to send high-definition images in real time for what the surgeon will be intervening. At the end of it, the device is removed and the small incision is closed.
Endoscopic spine surgery can be used for herniated discs, arthropathies, sciatica, and stenosis. It is performed only when the resources of an adequate administration of spinal injections or physiotherapy have been exhausted.